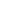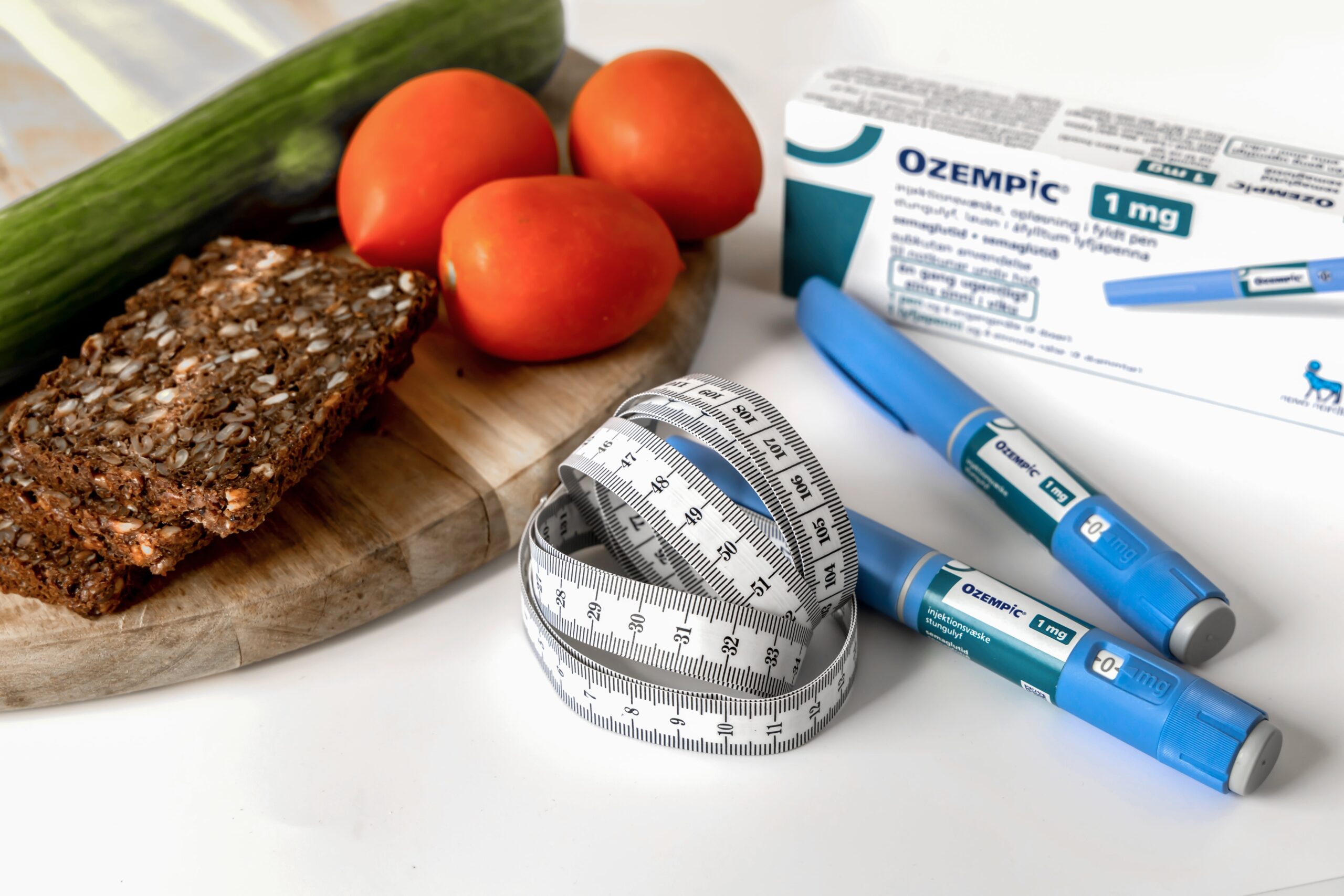
Drugs for weight loss such as Ozempic are becoming so popular that employers are now cutting off workers’ access to insurance coverage for the drugs to mitigate climbing bills.
Spending regarding the drugs, which may cost up to $1,350 per month for patients, is now reaching eight-digit spending regarding insurance plans. These costs are straining plans’ finances, including plans which employers fund.
The University of Texas said it was ending insurance coverage regarding Saxenda and Wegovy, made by Novo Nordisk, for people that its health plans cover effective as of September 1. The decision came after its costs regarding these drugs increased by over three times in the last 18 months, reaching $5 million in spending per month.
A university newsletter stated that paying for these medicines is “unsustainable” because of the rate of expenditures on prescription drugs. The newsletter stated that continuing to cover the drugs would add $73 million per year to prescription plans, driving premiums for all employees up by up to 3 percent.
3,200 workers, representing about 3 percent of the university’s workforce, have been using insurance coverage for Saxenda or Wegovy prescriptions.
The cuts in reimbursements, in addition to some employers’ other restrictions, signify a downside to the medical success of the drugs. While these drugs have helped people lose quite significant amounts of weight, employers who need to pay for the drugs might not have the capacity to afford paying for them.
The usage of drugs like Wegovy and Ozempic has become extremely popular because of word of mouth regarding their ability to induce weight loss. Demand for the drugs has gotten so high, so quickly, that the drugs’ maker, Novo Nordisk, has not been able to make enough of the drugs. Analysts have been revising their sales estimates for the drugs upward.
Morgan Stanley’s analysts had previously forecast an estimate of a $23 billion worldwide anti-obesity market. Last month they increased that estimate to $77 billion.
The quickly increasing popularity of these drugs is causing companies to be confounded. Companies might want to help their employees who are extremely overweight and might develop medical conditions as a result which add to their costs of health insurance, but employers worry about adding costly new expenses.
The University of Texas, in a newsletter, stated it is not seeing reductions in costs for health conditions which might be caused by excessive weight, stating that the “excessive cost” of weight loss drugs is leading to savings not being seen.
The changes in reimbursements affect drug coverage when the drugs are being used for weight loss. The changes aren’t affecting coverage when the drugs are being used for diabetes. The drugs are part of a class of drugs which function by mimicking gut hormones known as GLP-1.
Ascension Healthcare operates Catholic and nonprofit hospitals, as well as other facilities in multiple states, mostly in the South and Midwest. The employer, which employs almost 140,000 people, ceased coverage for anti-obesity medications including Saxenda and Wegovy for health plan members as of July 1. This exclusion also includes older drugs for weight loss like phentermine.
The list price from Novo Nordisk, which is based out of Denmark, is $1,349 for about one month’s supply of Saxenda or Wegovy. Ozempic is a related medication. It is approved for the treatment of diabetes. It costs around $930 per month. Ozempic isn’t usually covered by insurance for weight loss regarding those who don’t have diabetes.
No generic versions are currently available of semaglutide drugs such as Wegovy and Ozempic.
The cutbacks in coverage might reverse or stall progress that doctors and employees have made recently regarding obtaining reimbursement from health insurance of weight loss prescriptions. An increasing number of health plans were agreeing to cover the medications as research was showing obesity is a disease and not a lifestyle choice.
Some employers still cover the medications, but have done things to attempt to lower costs. The University of Michigan has increased Saxenda and Wegovy’s monthly copay from $20 to $45.
This decision was intended to encourage members of health plans to first try options which are less expensive, such as phentermine, which has a $10 per month copay. About 120,000 are covered by the university’s health plans.
Connecticut’s drug plan for employees of the state government now needs members to get anti-obesity medications through an anti-obesity practice that is state-based known as Intellihealth. Intellihealth offers app-based care as well as telehealth-based care.
Connecticut’s costs for GLP-1 medications for members of plans have gone up 50 percent since 2020. The costs are on pace to reach $30 million every year by the end of 2023.